Pain management has become a public health priority. To this end, various national recommendations and laws have been passed to improve the quality of care. With 70% of patients concerned, acute pain is the main reason for consultation in France. In emergency medicine, this reality is well known as it represents more than half of all admissions. However, even though it is the most frequently reported symptom, the treatment of this distressing element sometimes takes a back seat due to the saturation of the service, the lack of staff or the protocols for administering sedatives. What if there was a practical and flexible non-drug solution to relieve pain in the emergency department? Let’s find out.
Pain in the emergency department: a common symptom
According to the Pain Management and Tracking in the Emergency Department, acute pain is no stranger to patients, affecting between 50 and 80% of visits. However, in addition to being deeply unpleasant, pain is also harmful to the body, hence the importance of early management.
When waiting adds to patients’ ailments
When faced with painful sensations, we all tend to develop scenarios in which the severity of our ailments becomes catastrophic. During a prolonged waiting phase, the imagination runs riot and the patient concentrates mainly on his or her perception of pain, which does not help to dispel it.
The hospital environment unwillingly contributes to the worsening of this impression. Most visitors anticipate the care that awaits them, imagine the possible complications and often fear the diagnosis: “What will the doctor tell me?”; “Will I have to wait much longer?”; “How many more patients before I am treated?”; “Will my injury aggravate over time?”; “My pain is way worse than it was 5/10/20 minutes ago, is this normal?”.
These chain questions are obviously legitimate, but focusing on the subject never alleviates the suffering and fears. In the bustle of the ward, the carers unfortunately do not always have the time and staff to reassure each patient individually.
Coping with organisational pressure and protocolisation
Illness, trauma, contusion, laceration… Overworked emergency departments deal with patients suffering from painful ailments and anxiety on a daily basis. Unlike other hospital care, the medical team must react quickly, sometimes in complex conditions.
The reasons for admission to the emergency room are extremely varied, as are the causes of the pain. On arrival in the department, the patient is assessed and then oriented according to the seriousness of his or her pathology. This evaluation depends on several parameters:
- haemodynamic ;
- respiratory ;
- neurological ;
- pain intensity.
Despite all the coherence and necessity of this procedure, it does not occur in a twinkling of an eye and cannot be rushed. Thus, the flow of patients sometimes causes major congestion in the department. Organisational pressure and protocolisation therefore have a strong influence on individualised care and pain management, as shown by the study on the management of acute pain in adult emergency medicine.
Furthermore, practice surveys reveal that pain management and traceability are not always automatic. According to the file Management and traceability of pain in the emergency patient, less than “half of patients with pain are treated”.
To meet the demands, the administration of morphine remains the main treatment in emergency facilities. Emergency physicians are increasingly using local anaesthesia, but this requires established protocols that make the treatment more cumbersome… Now, caregivers have another non-pharmacological analgesic method to rely on.

Virtual reality: a useful non-medicinal complement to improve the quality of care
1. A practical and flexible device in the hospital
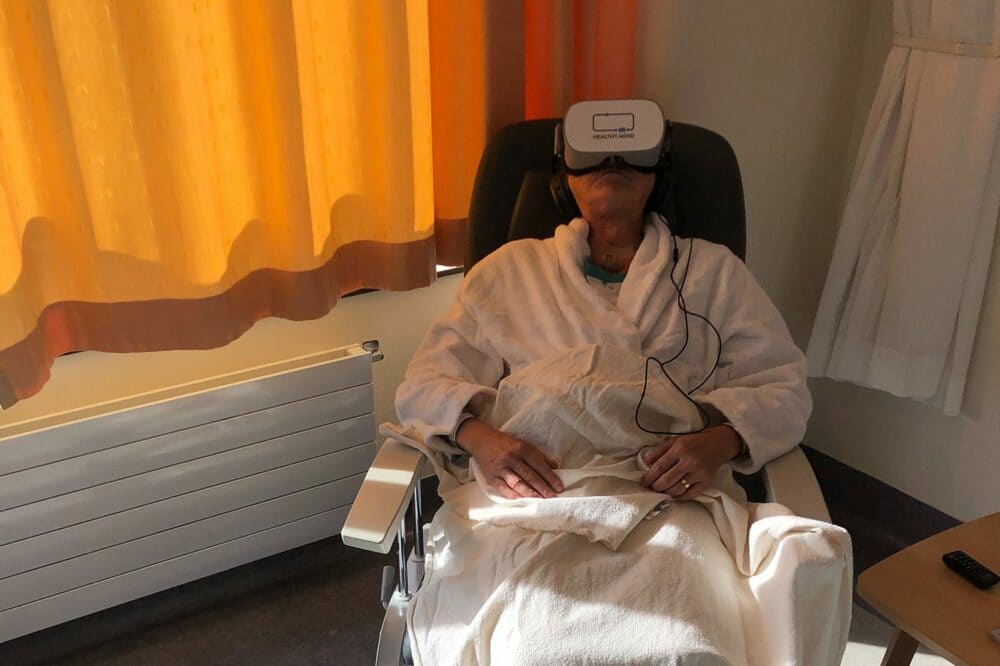
Among the solutions to defuse fear or anxiety, distraction remains strongly recommended by many studies, especially in paediatrics. Indeed, immersion in virtual reality directs the user towards a landscape designed to bring tranquillity and calm.
The Healthy Mind’s headsets leave the cables behind to allow the patient to move freely and adapt to the various hospital measures: procedures involving needles, venipunctures, lumbar punctures, infusions, burns or wounds (1st to 3rd degree). The versatility of the immersions makes them relevant in several sensitive configurations:
- psychiatric emergencies to reduce the anxiety of a patient in the throes of disorientation;
- gynaecological and maternity emergencies in order to relax and decrease the stress linked to an unexpected birth;
- paediatric emergencies to soothe parents whose child is being cared for, or to offer escape sessions when the child needs to be immobilised.
Thus, whatever the position, the device accompanies without constraining, as one carer testified:
“Use is facilitated with an easy-to-access interface and a mode that can be adapted according to the needs in time and in contemplative or interactive mode for people who require mobility.”
The treatment of pain must be adapted to its intensity, to the patient and to the pathology. The advantage of virtual reality is that it is just as effective with a person with no previous history as with a child, a pregnant woman or an elderly person, since there are no contraindications to its use.
Moreover, patients are generally curious and intrigued by the device:
“The innovative approach was appreciated, as it aroused interest as well as curiosity and its use in an emergency department gave confidence to patients looking for non-drug means of pain management.”
2. Fully customisable software
If there is one department where adaptability is a must, it’s the emergency department. There is no need for a complicated and time-consuming software to be installed. For that reason, Healthy Mind incorporates practical features that meet the challenges of the hospital: adjustable immersion times.
In addition, the device incorporates other functionalities to ensure the continuity of the link between the patient and the carer so that communication remains possible at all times. The implementation of virtual reality in the department doesn’t require staff training and can therefore be introduced quickly to relieve patients, without immobilising the carers.
3. Proven effectiveness in relieving pain in the emergency department
Until now, opioid drugs have been the first line of treatment for acute pain in the emergency department. Although in some cases, this administration is unavoidable, the fact remains that certain non-pharmacological actions can complement the analgesic effect, or even favour recourse to a locoregional rather than general anaesthesia.
Among them, virtual reality presents a multisensory approach that combines the benefits of several therapeutic solutions such as hypnosis, music therapy or cardiac coherence:
“Virtual reality goggles have allowed a modification of the painful perception for several patients when using it.”
In addition to reducing suffering, the simulations also act on patients’ feelings of anxiety and fear, as shown by the results of the study published in the journal BMC Emergency Medicine:
- 50% reduction in anxiety;
- 33% reduction in pain;
- good tolerance of virtual reality simulation;
- high user satisfaction.
To relieve pain in the emergency department is a fundamental issue as most patients experience it during their stay in hospital. Thanks to a non-medicinal approach, virtual reality offers a complementary therapeutic solution that requires little congestion and mobilisation of staff. With a notable reduction in anxiety and pain, the device can even demonstrate its usefulness in other use cases and thus reveal its full relevance in the hospital environment. Since a picture is often worth a thousand words, we invite you to discover our headsets during a demonstration.







