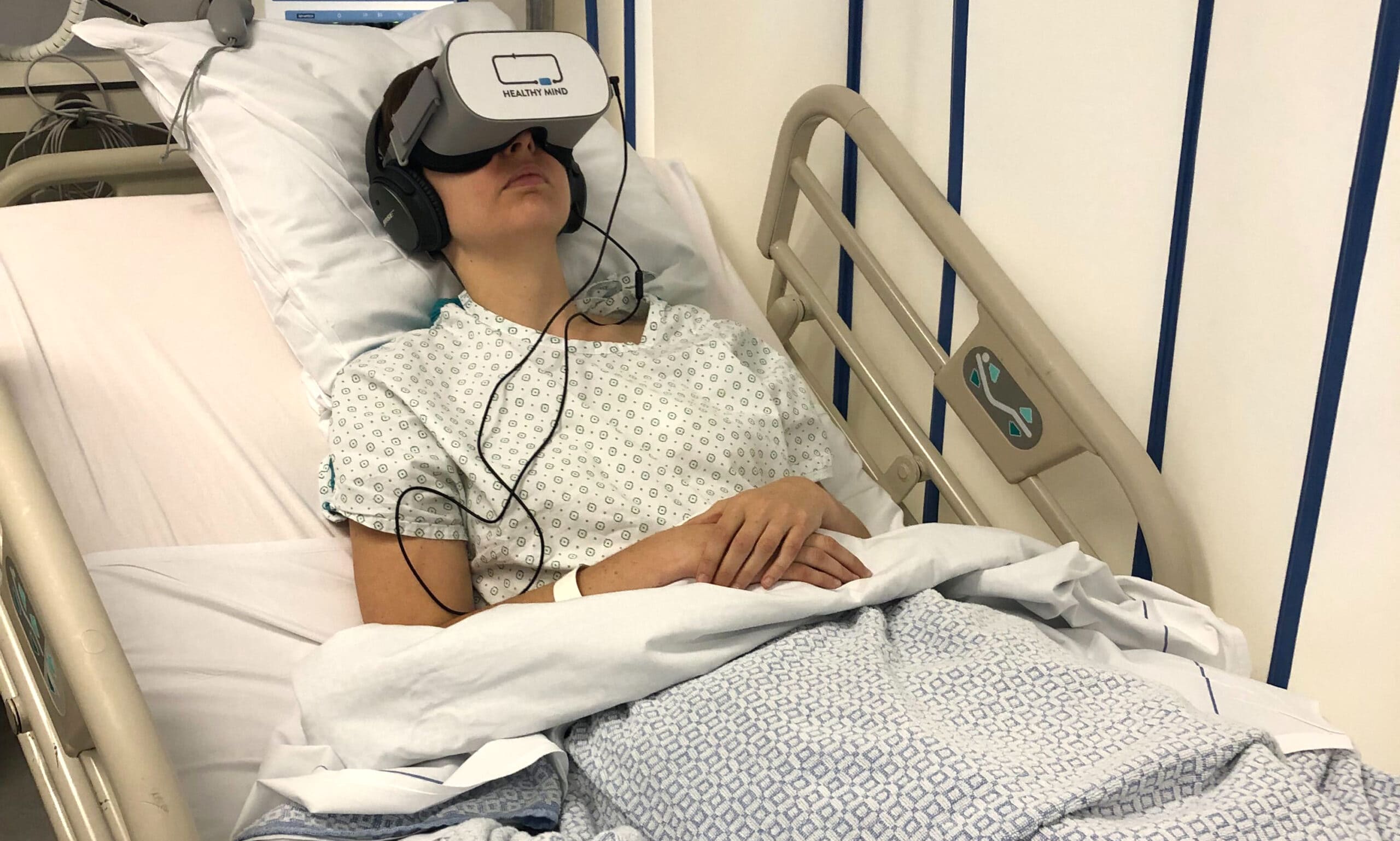
Relying on the benefits of therapeutic virtual reality in the post-anesthesia care unit (PACU)
According to the French Society of Anaesthesia and Intensive Care (Sfar), more than 13 million anaesthesias are performed each year in France. Despite the frequency of this medical procedure, anaesthesia is often accompanied by anxiety and fear. After an operation, patients are placed under the supervision of a nursing team in the post-anesthesia care unit (PACU). This stage serves as a transition to regain strength and eliminate sedative drugs before going home. The use of virtual reality in the recovery room after a painful or anxiety-provoking procedure offers many benefits to soothe patients. What are they? We propose to discover 3 major aspects that make this technology a precious ally in postoperative recovery.
Reducing patient stress and facilitating recovery in the recovery room
The post-anesthesia care unit (PACU) or recovery room is a mandatory step in the vast majority of situations after an operation under general or local anaesthesia for a therapeutic or diagnostic procedure. Depending on the type of surgery, the medical team may have to check the respiratory, cardiac and renal functions, the wounds, the dressing and any drains that may have been put in.
Although this phase is of essential interest in the medical pathway, this intensive care unit can be a source of anxiety for patients because of the postoperative context and environment.
Furthermore, various studies suggest that a high level of pre-operative anxiety makes post-operative recovery slower, more complicated and painful. Thus, by acting on this factor, recovery in the post-anesthesia care unit will be greatly improved. The Healthy Mind therapeutic virtual reality headsets allow us to act on this lever and reduce anxiety before the operation.
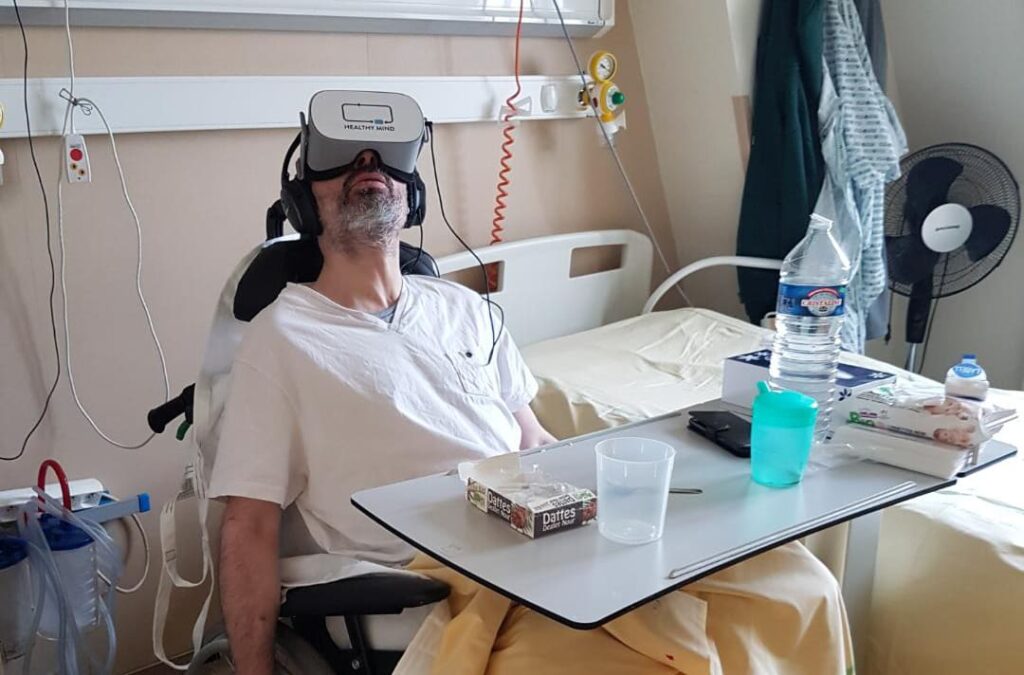
Improving patient comfort after surgery
The notion of comfort in the post-anesthesia care unit is multidimensional as it concerns the physical, psychosociological and environmental aspects. One of the first sources of nuisance in the recovery room concerns the surrounding noise, particularly the monitoring sound indicators. In addition to being disturbing, these signals remind patients of the environment in which they are located, which can generate additional discomfort or stress.
Through virtual reality immersion, the patient is immersed both visually and aurally in a landscape designed to relax them. In addition, Healthy Mind’s creations rely on the principles of music therapy to add a calming dimension to the experience. For example, the use of sound helps to relax and reduce anxiety.
Physical discomfort manifests itself as pain, nausea or hypothermia. The analgesic action of therapeutic virtual reality is then used to relieve the patients’ disturbing symptoms. Indeed, several studies have demonstrated this surprising effect, notably that of the team of Mosso Vázquez J.L., Wierderhold B.K., Miller I., Mosso Lara D. and Wierderhold M.D. The latter observed a significant reduction in the perception of pain (-22%) and visceral response (-8% respiratory rate, -32% salivation) in the group using virtual reality during an upper gastroscopy. Other clinical studies confirm this observation.
Furthermore, the design of virtual reality software is based on a teleportation principle to avoid the appearance of cyberkinetosis, the virtual motion sickness. Thus, there is no risk that the aches and pains felt before immersion will be amplified or worsened by the use of this technology.
Finally, promiscuity or lack of privacy can also be a source of discomfort. While immersion cannot materially change the situation, it does allow the patient to turn their attention away from these distracting elements and focus on a more relaxing experience. By abandoning the anxiety-provoking aspects, immersion offers a way to refocus on oneself.
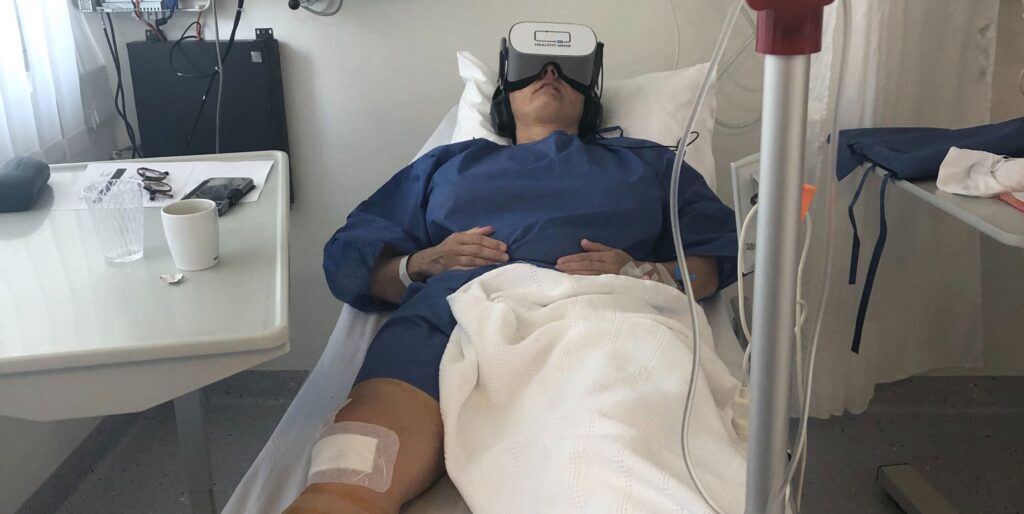
Reducing post-operative pain
Patients usually feel uncomfortable and on guard after surgery. However, anxiety not only leads to an unpleasant experience, it can also mean an increase in pain sensation. Dr Oberle and his team have found a link between postoperative anxiety and pain. In order to reduce the suffering experienced, additional treatment may be necessary. In this case, the non-pharmacological approach is an indispensable first option in order to reduce the possible side effects of medication.
A study published in the British Journal of Surgery estimates that the risk of complication or even re-hospitalisation in patients suffering from anxiety is +20%. These data confirm the importance of taking care of pre- and postoperative psychological health, particularly in the post-operative recovery room.
The Bicetre AP-HP hospital in Paris offers Healthy Mind’s therapeutic virtual reality headsets to patients undergoing lithotripsy in the hepato-gastroenterology department. This operation consists of breaking up a patient’s stones so that they can be eliminated through the urine.
Although the procedure only takes 30 to 40 minutes, it is relatively painful. As a result, patients can inject a dose of morphine sedation on demand (capped) using a pump provided.
The introduction of virtual immersion has had striking effects:
- morphine consumption has decreased by 50%;
- hospitalization time has decreased by 50%, leading to an improvement in the flow of patients in the recovery room and in ambulatory care;
- the number of patients treated in one morning for lithotripsy has doubled.
Thus, virtual reality offers a first-rate non-pharmacological solution for limiting medication and hospitalization time. On the other hand, its use allows the medical teams to take care of more patients without neglecting the quality of care.
With reduced anxiety, improved comfort, faster recovery and fewer postoperative side effects, virtual reality in the recovery room has its place! Immersions promote a more peaceful experience of hospitalization, without causing side effects for patients. With numerous applications, the device offers undeniable medical and therapeutic benefits for the patient, as well as significant savings in time and money for health establishments. We would be delighted to discuss the implementation of this solution or to offer you a demonstration, feel free to contact us.
Sources:
- French Society of Anesthesia and Resuscitation;
- Lang, E-V. (2002). Cost analysis of supplemental hypnosis with sedation in outpatient interventional radiology procedures. Radiology, 222(2), 375-38;
- Observational results observed by the team at the Bicetre Hospital AP-HP in Paris over a 3-month period (2020-2021);
- Johnston M, Carpenter L. Relationship between pre-operative anxiety and post-operative status. Psychol.Med. 1980; 10: 361-7;
- Kain ZN, Sevarino F, Pincus S et al. Attenuation of the preoperative stress response with midazolam: effects on postoperative outcomes. Anesthesiology 2000; 93: 141-7;
- Kain ZN, Sevarino F, Alexander GM, Pincus S, Mayes LC. Preoperative anxiety and postoperative pain in women undergoing hysterectomy. A repeated-measures design. J Psychosom.Res. 2000; 49: 417-22;
- British Journal of Surgery (BJS) 14 February 2017 DOI: 10.1002/bjs.10474 Association between psychological health and wound complications after surgery.