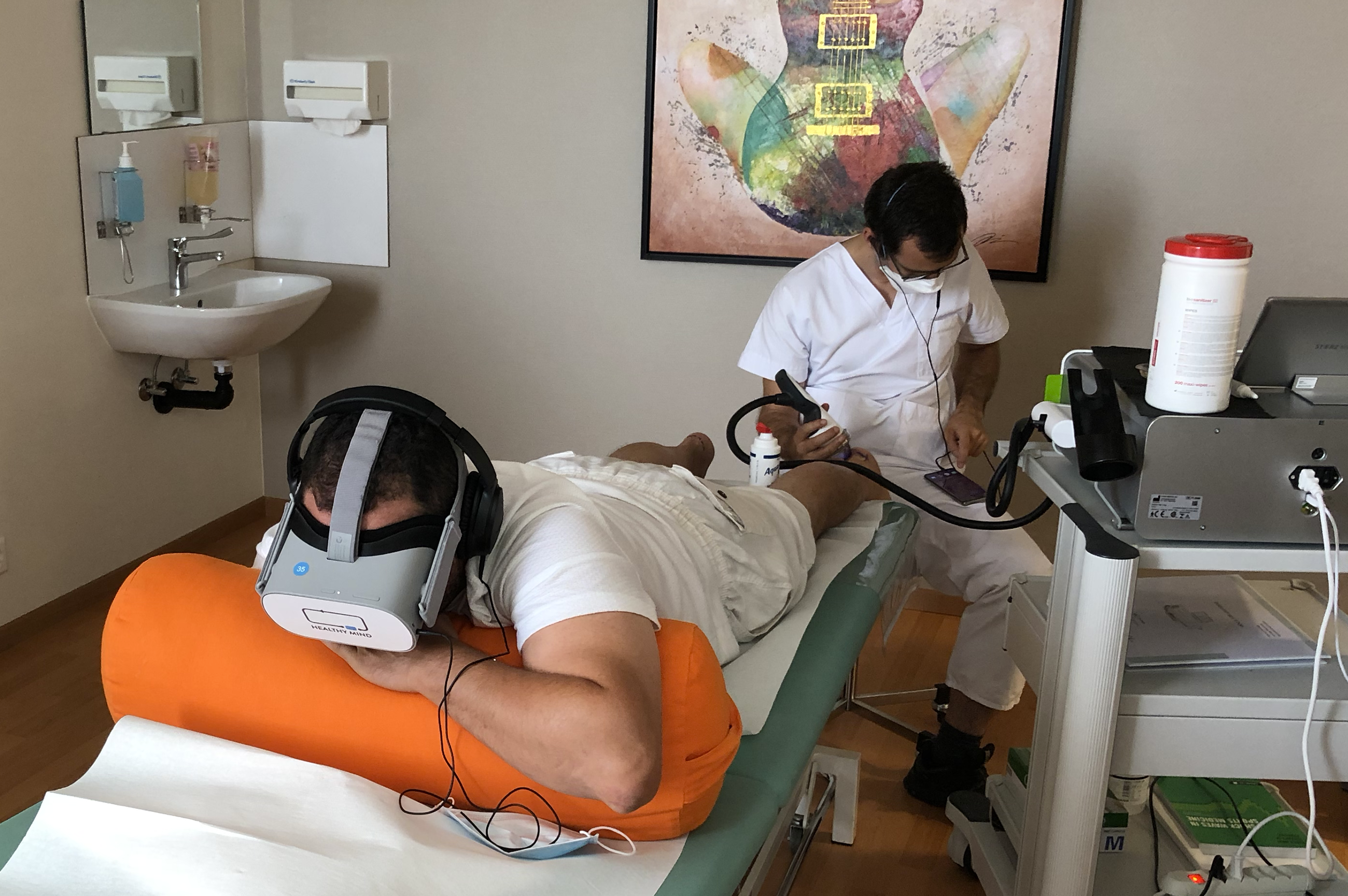
According to Inserm (National Institute of Health and Medical Research), pain is the cause of almost 2/3 of all medical consultations. Because of its omnipresence, this unpleasant sensory and emotional experience is the subject of numerous studies aimed at thwarting its mechanisms. Among non-pharmacological treatments, therapeutic virtual reality offers an effective response to pain management. How does it work? In this article, you’ll discover why this revolutionary technology is transforming the medical landscape and delivering tangible relief to sufferers of both chronic and acute pain.
Diverting attention: an effective painkiller
The more we focus on a painful sensation, the more important it becomes. In a study on pain catastrophizing, researchers identified three main components of this phenomenon: rumination, amplification and powerlessness. As a result, people with negative pain-related thoughts experience greater emotional distress and higher intensity than others.
How can we help patients put things into perspective and encourage them to relax? To address this issue, numerous scientific studies have focused on the positive role of attention detour in reducing pain perception.
The review How do attention and emotion influence pain processing? examined several studies on the role of attentional distraction in pain reduction. It concluded that attention directed towards non-painful or pleasant stimuli can influence pain perception.
Another study used functional magnetic resonance imaging (fMRI) to explore the neural mechanisms underlying the effect of distraction on pain. The results reveal that when participants’ attention is diverted to a cognitive task requiring high concentration, the brain regions involved in pain perception are less activated.
Taken together, these findings highlight the importance of attention detour in pain modulation. By focusing attention on distracting stimuli or cognitive tasks, patients are able to reduce their perception of pain, without the addition of medication.
However, how can this process be initiated when the person is in an anxiety-inducing environment such as a hospital, or when intrusive thoughts inhibit the activation of this mechanism?

Studies showing how virtual reality reduces pain
Therapeutic virtual reality is becoming increasingly popular in the healthcare field for pain relief, and not without good reason. Several scientific studies have been conducted to explore the analgesic effects of this device.
One study involved teenagers undergoing painful medical procedures following burns. Caregivers noted a reduction in pain and anxiety during treatment thanks to the use of virtual reality. Another study by Hoffman and his team showed that the detour of attention offered by immersion significantly reduced pain in burn patients.
Another experiment involved patients undergoing cardiac surgery. Some were exposed to virtual reality environments during the post-operative period, while others received standard care. Results revealed that patients using virtual reality reported a significant reduction in pain and a decrease in analgesic intake.
A systematic review of several clinical trials investigated the use of virtual reality as a distraction for pain relief. The results of this analysis indicated that virtual reality significantly reduced pain in patients suffering from a variety of conditions, including burns, chronic pain and invasive medical procedures.
Finally, another review examined various studies on the use of virtual reality for pain control. It highlights possible mechanisms by which virtual reality acts on pain, including diverting the patient’s attention from the painful sensation, inducing a state of relaxation and reducing anxiety.
Taken together, these studies conclusively suggest that the use of virtual reality can alleviate pain in a wide range of medical contexts. This technology offers a promising non-pharmacological approach to pain management. See our clinical studies for further demonstrations of the effectiveness of therapeutic virtual reality.
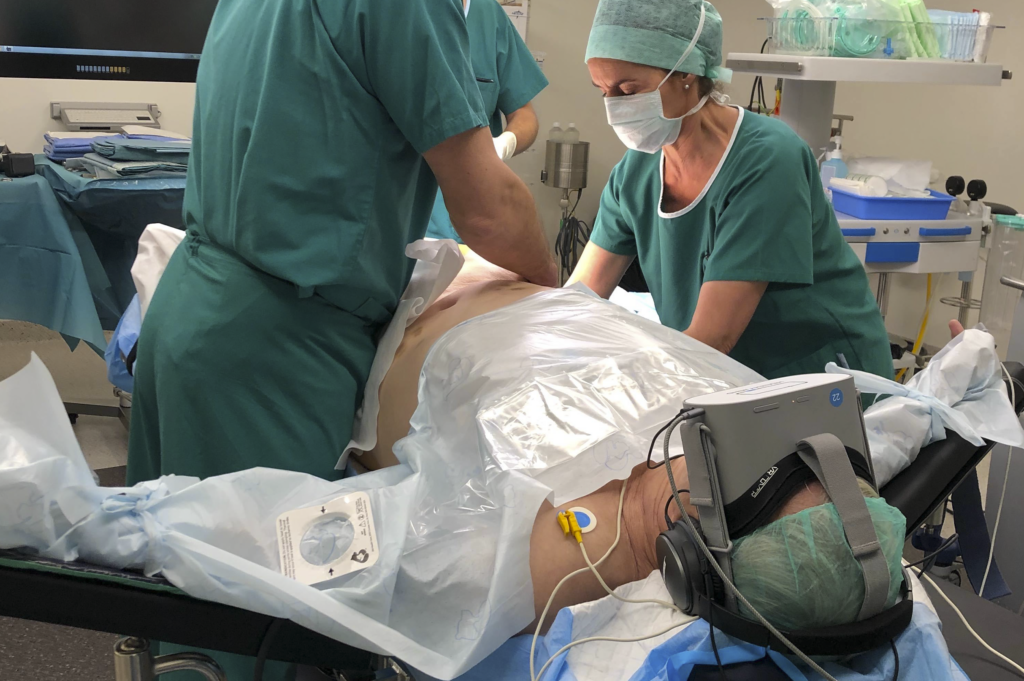
Combining several analgesic principles in a single device
By combining several relaxing principles that serve to divert attention, therapeutic virtual reality offers a coherent, reliable and relevant response to soothe patients’ pain in a variety of hospital settings, as Marie-Charlotte Desmaizieres, anaesthetist and referent of the Hypnosis Institute at Paris Saint-Joseph Hospital, where our Healthy Mind medical device is used for colonoscopies, points out:
“The effect goes beyond simple diversion, with some people achieving a very deep state of relaxation. Overall, we are able to reduce or even eliminate sedation and reduce the duration of post-intervention monitoring.”
So what are the complementary techniques that make the Healthy Mind device so effective?
1. Medical hypnosis
Medical hypnosis is based on an altered state of consciousness that helps the patient to relieve pain. Several mechanisms are involved in achieving this analgesic effect.
Pain is often accompanied by an intense emotional response, such as anxiety, fear or tension. Medical hypnosis helps to modify this emotional response by inducing a state of relaxation, calm and well-being. By regulating the negative emotions associated with pain, hypnosis enables the patient to cope better with pain and experience it less intensely.
On the other hand, hypnosis induces a state of deep relaxation and intense concentration that serves to divert attention from the pain and perceive it differently. Hypnotic suggestions modify the way the brain processes pain signals, acting on their amplitude or filtering them out.
Finally, hypnosis can stimulate the release of endorphins, natural substances produced by the body to relieve pain. By inducing a hypnotic state, it is possible to activate these endogenous mechanisms and increase endorphin secretion, thereby helping to reduce the pain felt by the patient.
2. Music therapy
Music therapy is a therapeutic approach that uses melody to treat a variety of health problems, including pain. Notes have the surprising power to divert attention from pain by providing pleasant auditory stimulation. So, by focusing on the music, patients can reduce their attention on the painful stimulus.
On the other hand, listening to harmonious sounds stimulates the release of neurotransmitters such as dopamine, a molecule associated with pleasure and well-being. This activation of the reward system helps to reduce pain and improve patients’ mood.
In this way, relaxing music helps to reduce stress and anxiety, which are often associated with pain. By promoting a state of relaxation, music therapy helps release muscular tension.
In addition, music therapy can stimulate the release of endorphins, the body’s natural painkillers, leading to a reduction in pain levels.

3. Cardiac coherence
Cardiac coherence is a technique that aims to regulate heart rate by controlling breathing. The practice involves slow, deep, regular breathing that promotes activation of the parasympathetic nervous system. This system is responsible for the body’s relaxation response. As a result, stress, anxiety and muscle tension associated with pain are reduced.
By promoting the dominance of the parasympathetic system, cardiac coherence modulates pain-related physiological responses, such as increased heart rate and blood pressure.
The practice of cardiac coherence increases heart rate variability, i.e. the variations between successive heartbeat intervals. This process is associated with good health and greater ability to cope with stress. As demonstrated by the study on pain catastrophization mentioned above, this relaxation contributes to better pain management.
Thanks to its practical, ergonomic design, the Healthy Mind solution can be adapted to different practices and patients, guaranteeing a high-quality, immersive experience. For more information on our device or to test the equipment, please contact our team.
Sources :
- Villemure, C., & Bushnell, M. C. (2002). Cognitive modulation of pain : How do attention and emotion influence pain processing? Pain, 95(3), 195–199.
- Sullivan, M. J. L., Bishop, S. R., & Pivik, J. (1995). The Pain Catastrophizing Scale: Development and validation. Psychological Assessment, 7(4), 524–532.
- Bantick SJ, Wise RG, Ploghaus A, Clare S, Smith SM, Tracey I. Imaging how attention modulates pain in humans using functional MRI. Brain. 2002 Feb;125(Pt 2):310-9. doi: 10.1093/brain/awf022. PMID: 11844731.
- Belinda Kipping, Sylvia Rodger, Kate Miller, Roy M. Kimble. Virtual reality for acute pain reduction in adolescents undergoing burn wound care: A prospective randomized controlled trial, 17 November 2011.
- Hoffman HG, Patterson DR, Carrougher GJ, Sharar SR. Effectiveness of virtual reality-based pain control with multiple treatments. Clin J Pain. 2001 Sep;17(3):229-35. doi: 10.1097/00002508-200109000-00007. PMID: 11587113.
- Mosso-Vázquez JL, Gao K, Wiederhold BK, Wiederhold MD. Virtual reality for pain management in cardiac surgery. Cyberpsychol Behav Soc Netw. 2014 Jun;17(6):371-8. doi: 10.1089/cyber.2014.0198. PMID: 24892200; PMCID: PMC4043366.
- Malloy KM, Milling LS. The effectiveness of virtual reality distraction for pain reduction: a systematic review. Clin Psychol Rev. 2010 Dec;30(8):1011-8. doi: 10.1016/j.cpr.2010.07.001. Epub 2010 Jul 13. PMID: 20691523.
- Mahrer NE, Gold JI. The use of virtual reality for pain control: a review. Curr Pain Headache Rep. 2009 Apr;13(2):100-9. doi: 10.1007/s11916-009-0019-8. PMID: 19272275.