On a daily basis, anxiety contributes to a decreased quality of life for palliative care patients. Depending on its duration and intensity, the treatments considered to relieve it vary. When the sufferer is not obsessive, anxiety disorders do not require the systematic prescription of an anxiolytic. In these mild to moderate cases, non-medicinal pain treatments can be used to provide a safe, reassuring and positive environment. So, as a carer or a relative of the patient, how can we detect the warning signs and what tools can we use to alleviate uneasiness? This article explores the assessment of stress symptoms and therapeutic techniques for managing anxiety in palliative care.
Identifying signals of anxiety in the terminally ill
Distinguishing anxiety attacks from the physical and psychological symptoms of an illness is a complex task. Nevertheless, there are clinical manifestations that allow us to understand these phenomena and to identify them. What are they?
Somatic manifestations of stress
Anxiety is expressed by physical symptoms that give evidence of a neurovegetative dysregulation, i.e. a disturbance in the control and regulation of the body’s major functions. Several somatic symptoms are thus associated with disquietude:
- respiratory signals: sensation of constriction, chest tightness or dyspnoea (breathing discomfort).
- cardiovascular indicators: palpitations, tachycardia, atypical chest pain or lipothymia (temporary feeling of faintness without loss of consciousness).
- neuromuscular clues: tenseness, cramps, tremors, motor restlessness, paraesthesia (disturbance of the sense of touch), tinnitus or dizziness.
- digestive signs: loss of appetite, nausea or colonic spasms.
- increased expression of or unexplained change in pre-existing pain.
- the appearance of increased fatigue and sleep disorders.
Psychological symptoms of anxiety
Patients are not always aware of their state of anxiety, and even when they are, the expression of their feelings may be hindered by shame, denial or the desire to protect their family. However, stress can still be observed and generally manifests itself in three ways:
- affective: worry, dramatised anticipation of future events, fears of undetermined consequences, excessive fear, feeling of loss of control, increased feeling of powerlessness.
- cognitive: difficulty concentrating, rumination, tendency to forget, thought blocking.
- behavioural: distrust, irritability, hypervigilance, mental or motor agitation.
Factors contributing to an anxiety disorder
In a context of increased vulnerability, sadness or fear, patients are all the more sensitive to their environment. Anxiety can therefore be contagious. If the patient initially had a good tolerance threshold, it is not rare for his apprehension to be increased by the anxious decompensation of his relatives or medical and nursing staff.
The approach of death, whether real or not, often leads to an inner struggle and a reassessment of one’s existence. Questions arise, the loss of control increases, and sometimes an unconscious struggle with religious values or fundamental life conflicts arises.
An underlying psychiatric illness such as depression is a particularly aggravating factor for anxiety disorder. Drug reactions (withdrawal, corticosteroids) or poorly controlled pain provide a suitable nest for the patient’s stress to grow.
How screening scales help managing anxiety in palliative care
Identifying anxiety is the first step to treating it. A number of materials have emerged to diagnose and handle psychological distress. Two tools predominate in the hospital setting: the ESAS scale and HADS.
The ESAS scale: a screening tool for well-being in hospital
Developed by the Edmonton Palliative Care Team in Canada, this systemic scale called the Edmonton Symptom Assessment System (ESAS) provides an interdisciplinary approach to assessing the most common symptoms: pain, fatigue, nausea, depression, anxiety, appetite, sleepiness, dyspnoea and well-being.
On their own initiative or with the help of the nursing staff and the family, the patient checks the level for each category that corresponds to their perception of their condition. The ESAS provides a global view for the medical profession thanks to a graph summarising the answers. It is a quick test in the form of a self-questionnaire that estimates the stability of the situation and, if repeated, its development.
The HADS scale: the most used in palliative care
Established for patients with somatic diseases, the Hospital Anxiety and Depression Scale (HADS) is a self-assessment tool designed to detect anxiety and depressive disorders. It consists of 14 items rated from 0 to 3. Of these, seven questions concern anxiety and seven others focus on the depressive dimension. Interpretation depends on the final score obtained out of 21 points:
- 7 or less: no symptoms;
- 8 to 10: possible anxiety;
- from 11 points: probable anxiety disorder.
Non-drug treatments for pain to improve the patient’s quality of life and comfort
When agitation is not incapacitating, non-drug interventions are preferred to relieve patients. This end-of-life comfort care can also be combined with pharmacological approaches in cases of severe anxiety.
Referring to a psychologist to manage anxiety attacks
As part of a multidisciplinary approach, the psychologist focuses on the psychic, subjective and relational aspects of the suffering person. By establishing a trusting relationship, the professional offers an attentive and empathetic ear, supports and advises, but above all leads the patient to identify and express his or her emotions.
This in-depth communication work awakens and sheds light on dormant pathologies. The psychologist then becomes a pillar for the care team and for the relatives: he/she brings understanding of the situation to the former and sensitivity to the latter. Only the patient’s refusal is a contraindication.
Exploring the Toucher-Massage® technique
As a genuine support tool, gentle forms of massage help to reduce patients’ torments. The concept of Toucher-massage® appeared in the 1980s to train and raise awareness among carers to well-being gestures. This technique leads hospitalized persons to a state of calm and relaxation through light pressure or kneading movements.
Controlled clinical trials have shown a significant reduction in anxiety disorders among people with oncological diseases. However, phlebitis, fever, inflammation or skin disorders are contraindications to receiving massages.
Using sophrology to promote relaxation
Sophrology invites you to become aware of your breathing, your emotions and your perceptions. Directly linked to relaxation and visualisation, this activity aims to harmonise the body and mind in order to achieve balance. It stimulates self-confidence, channels fears and facilitates a regaining of control over the body and its symptoms.
Clinical trials on the effectiveness of sophrology in palliative care are lacking. However, the analgesic and palliative care teams within the Department of Rehabilitation and Geriatrics of the University Hospitals of Geneva have observed a clear reduction in anxiety in the sufferers treated. Requiring the active participation of the patient, the contraindications to this practice are confusional states, personality disorders and advanced cognitive deficits.
Considering virtual reality for anxiety management in palliative care
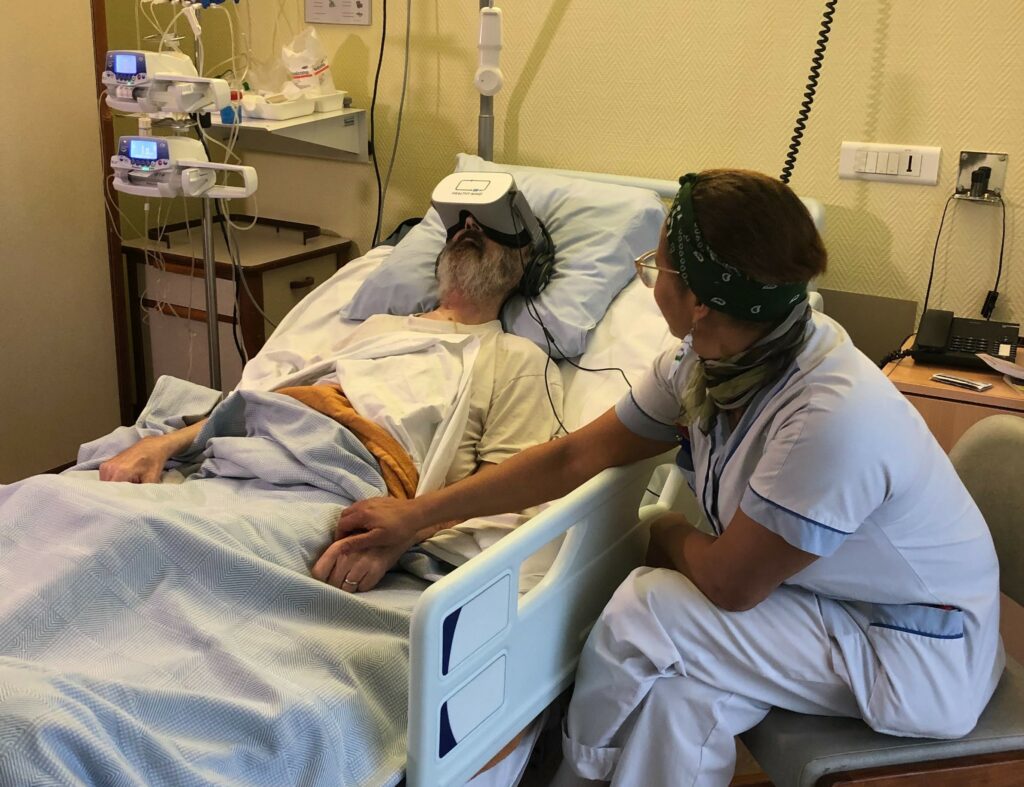
Virtual reality (VR) is based on 3D technology that allows the patient to be immersed in a virtual landscape. This technique has a non-pharmacological analgesic and anxiolytic effect. The relaxing environments are paired with principles of medical hypnosis, music therapy and cardiac coherence in order to maximise the therapeutic action.
The study by Erwan Gremion, Y. C., showed a 70% decrease in anxiety and pain after the Healthy Mind virtual reality session in patients in palliative care units. Immersion in VR is the therapy of choice for promoting well-being and has no contraindications if the person does not have epilepsy or advanced cognitive deficits.
As the end of life approaches, anxious emotions invade daily lives and express themselves in somatic and psychological symptoms. Faced with the distress of patients, non-drug treatments for pain allow caregivers and relatives to offer physical and mental relief. Among them, virtual reality immersion appears as a real support for managing anxiety in palliative care. To learn more about our solution, please contact our teams and ask for a demonstration of our virtual reality headset.
Sources:
- Nursing Diagnostics, Interventions and Relational Basis of Denges-Moorhoose, De Boeck University, Montreal: Ed.du Renouveau Pédagogique Inc. 2001, p. 144.
- Vignaroli E, Pace EA, Willey J, et al. The Edmonton symptom assessment system as a screening tool for depression and anxiety. J Palliat Med 2006;9:296-303.
- Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatrica Scandinavia 1983,67:361-70.
- Boegli and Cabotte, 2006, Controlled clinical trials on the anxiolytic efficacy of massage.
- Erwan Gremion, Y.C. Maison Pallia-Vie. Contribution of therapeutic virtual reality in the management of pain and anxiety for day care in palliative care.
- National Agency for Health Accreditation and Evaluation (ANAES). Management of adults in need of palliative care, December 2002.
- S. Pautex V. Toni P. Bossert H. Hilleret D. Ducloux J. Forestier E. Cabotte Y. Philippin H. Guisado N. Vogt-Ferrier. Anxiety in palliative care. Rev Med Suisse 2006; volume 2. 31735.